Tolosa–Hunt syndrome
| Tolosa–Hunt syndrome | |
|---|---|
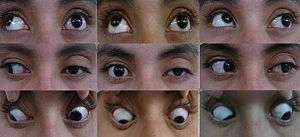 | |
| Neuro-ophthalmologic examination showing ophthalmoplegia in a patient with Tolosa–Hunt syndrome, prior to treatment. The central image represents forward gaze, and each image around it represents gaze in that direction (for example, in the upper left image, the patient looks up and right; the left eye is unable to accomplish this movement). The examination shows ptosis of the left eyelid, exotropia (outward deviation) of the primary gaze of the left eye, and paresis (weakness) of the left third, fourth and sixth cranial nerves. | |
| Classification and external resources | |
| Specialty | neurology |
| ICD-10 | G44.850 |
| ICD-9-CM | 378.55 |
| DiseasesDB | 31164 |
| eMedicine | neuro/373 |
| MeSH | D020333 |
Tolosa–Hunt syndrome (THS) is a rare disorder characterized by severe and unilateral headaches with extraocular palsies, usually involving the third, fourth, fifth, and sixth cranial nerves, and pain around the sides and back of the eye, along with weakness and paralysis (ophthalmoplegia) of certain eye muscles.[1]
In 2004, the International Headache Society provided a definition of the diagnostic criteria which included granuloma.[2]
Causes
The exact cause of THS is not known, but the disorder is thought to be, and often assumed to be, associated with inflammation of the areas behind the eyes (cavernous sinus and superior orbital fissure).
Signs and symptoms
Symptoms are usually limited to one side of the head, and in most cases the individual affected will experience intense, sharp pain and paralysis of muscles around the eye.[3] Symptoms may subside without medical intervention, yet recur without a noticeable pattern.[4]
In addition, affected individuals may experience paralysis of various facial nerves and drooping of the upper eyelid (ptosis). Other signs include double vision, fever, chronic fatigue, vertigo or arthralgia. Occasionally the patient may present with a feeling of protrusion of one or both eyeballs (exophthalmos).[3][4]
Diagnosis
THS is usually diagnosed via exclusion, and as such a vast amount of laboratory tests are required to rule out other causes of the patient's symptoms.[3] These tests include a complete blood count, thyroid function tests and serum protein electrophoresis.[3] Studies of cerebrospinal fluid may also be beneficial in distinguishing between THS and conditions with similar signs and symptoms.[3]
MRI scans of the brain and orbit with and without contrast, magnetic resonance angiography or digital subtraction angiography and a CT scan of the brain and orbit with and without contrast may all be useful in detecting inflammatory changes in the cavernous sinus, superior orbital fissure and/or orbital apex.[3] Inflammatory change of the orbit on cross sectional imaging in the absence of cranial nerve palsy is described by the more benign and general nomenclature of orbital pseudotumor.
Sometimes a biopsy may need to be obtained to confirm the diagnosis, as it is useful in ruling out a neoplasm.[3]
Differentials to consider when diagnosing THS include craniopharyngioma, migraine and meningioma.[3]
Treatment
Treatment of THS is usually completed using corticosteroids (often prednisolone) and immunosuppressive agents (such as methotrexate or azathioprine).[3] Corticosteroids act as analgesia and reduce pain (usually within 24–72 hours), as well as reducing the inflammatory mass, whereas immunosuppressive agents help reduce the autoimmune response.[3] Treatment is then continued in the same dosages for a further 7–10 days and then tapered slowly.[3]
Radiotherapy has also been proposed.[5]
Prognosis
The prognosis of THS is usually considered good. Patients usually respond to corticosteroids, and spontaneous remission can occur, although movement of ocular muscles may remain damaged.[3] Roughly 30–40% of patients who are treated for THS experience a relapse.[3]
Epidemiology
THS is uncommon in both the United States and internationally. In New Zealand, there is only one recorded case, there is also one recorded case in NSW Australia.[3] Both genders, male and female, are affected equally, and it typically occurs around the age of 60.[1]
References
- 1 2 "Tolosa–Hunt syndrome". Who Named It. Retrieved 2008-01-21.
- ↑ La Mantia L, Curone M, Rapoport AM, Bussone G (2006). "Tolosa–Hunt syndrome: critical literature review based on IHS 2004 criteria". Cephalalgia. 26 (7): 772–81. doi:10.1111/j.1468-2982.2006.01115.x. PMID 16776691.
- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 <Danette C Taylor, DO. "Tolosa–Hunt syndrome". eMedicine. Retrieved 2008-01-21.
- 1 2 "Tolosa Hunt Syndrome". National Organization for Rare Disorders, Inc. Retrieved 2008-01-21.
- ↑ Foubert-Samier A, Sibon I, Maire JP, Tison F (2005). "Long-term cure of Tolosa–Hunt syndrome after low-dose focal radiotherapy". Headache. 45 (4): 389–91. doi:10.1111/j.1526-4610.2005.05077_5.x. PMID 15836581.
| Wikimedia Commons has media related to Tolosa–Hunt syndrome. |